|
This observation highlights the need for ongoing retraining of techniques, even after the initial clinic visit. It has been noted that peak flow rates in individual patients tend to decrease over time, likely from waning skill and effort. In this situation, published tables of normal peak expiratory flow rates for height and weight are available. Of note, it is a common challenge in the inpatient setting that patients will not know their personal best. Respiratory therapy and nursing can easily obtain and report serial peak flow measurements throughout the hospital course to guide disposition decisions as well. A patient with a peak flow of less than or equal to 50% without improvement despite aggressive therapy should be admitted to the hospital for ongoing care and close monitoring for signs of impeding respiratory failure. Peak flow measurement is also useful in guiding disposition in the emergency setting. Some patients may be instructed to keep a supply of oral corticosteroids on hand to initiate therapy immediately. Patients usually activate their Yellow Zone plan, as well as escalate to either oral corticosteroid therapy and/or seek emergency care. Peak flow measurements in this range indicate that serious airway obstruction may be occurring and should be considered a medical emergency. Red Zone: Fifty percent or less of personal best. Action plans often contain reminders to the patient to look for and avoid, noxious stimuli such as fumes and second-hand smoke as well. Patients are typically instructed to employ their home action plan when they identify repeated readings in this zone. Standard action plans include increasing the dose and frequency of short-acting beta-agonist and possibly increasing the dose of inhaled corticosteroids. 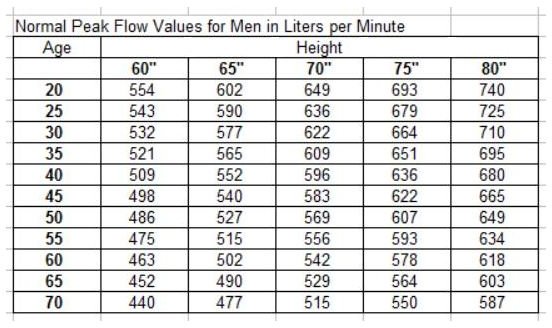
Yellow Zone: Fifty percent to 80% of personal best. No changes are needed to the present regimen. As long as no symptoms are present, the patient is considered at steady state. 
Green Zone: Usually set at 80% to 100% of personal best or normal peak flow. These should correlate with a written asthma action plan. For ease of patient interpretation, the colors of a traditional traffic light have been used to designate varying degrees of peak flow limitation. Typical peak flow meters are equipped with gauge markers indicating three “zones” that can be set by the patient or clinic staff to aid users in interpreting their peak flow scores. For those patients who are relatively well controlled and can sense worsening symptoms early in the course of an exacerbation, as-needed measurement is appropriate. For those patients who demonstrate a pattern of not having pronounced symptoms despite increasing disease activity, a clinician should outline daily (or more) measurement to identify deterioration rapidly and intervene appropriately. Specific instructions on how often and when an individual patient should be instructed to measure peak flow depends on patient characteristics and provider preference. It can be denoted on the meter to aid in interpretation. Typically, this number should be obtained during a period when the patient is feeling well and has just received maximal asthma therapy. 
Obtaining a “personal best” peak flow measurement during steady state for each patient is preferable to using published normal values, and this number should be used by both patients and clinicians to evaluate disease activity objectively. The most widely accepted use of peak flow measurement is in the daily and/or as-needed ambulatory evaluation of asthma.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
